France: Satelia, a remote monitoring system for those off the grid
The Satelia platform combines algorithms and people. The result is that many hospitalisations are avoided.
An innovation in the field
The interest of remote monitoring for chronic pathologies is obvious. But what about the 40% of patients who do not know how to use a digital tool? The Satelia platform, which was developed in the field, combines algorithms and people. The result is that many hospitalisations are avoided.
Made in cooperation with our partners from esanum.fr
About the contributor: Nicolas Pagès has just completed his internship in anaesthesia and intensive care at the Bordeaux University Hospital. In 2017, he put his medical studies on hold to co-found Satelia, of which he is the CEO. This remote monitoring platform now has more than fifty employees. Reimbursed by the French Social Security for its main indication, Satelia makes it possible to schedule a consultation at the right time and reduce the number of hospitalisations.
I am convinced that when you come from the field, you have a strong legitimacy to propose a health innovation. The same goes for digital health solutions. In this case, the idea of creating a remote monitoring platform came from a frustration that I felt in the field, during my internships in ambulatory surgery. What is the point of offering quality care in an establishment if the follow-up does not follow? It appeared to me that postoperative monitoring was not optimal: often the follow-up consists of a call to the patient the day after the operation, then nothing more before the postoperative consultation.
You can't put a carer behind every patient, it's not economically pertinent. But when a knee prosthesis is fitted, saying to the patient "You will be home tonight at 6pm, we will call you tomorrow and in seven days you will see the surgeon again" seems insufficient. What happens in case of pain or complications? How to obtain information on the patient's progress? Satelia is the missing link that allows the patient to remain close to the care centre at all times, as if he or she were gravitating towards it.
Satelia does not replace the physician. Algorithms based on clinical symptoms or physiological parameters detect periods of risk when a consultation may be beneficial. The right consultation at the right time is invaluable in the context of medical deserts. Moreover, Satelia aims to avoid hospitalisations. The results of the study carried out as part of a thesis at the University of Bordeaux are positive.1

Satelia's indications, focused on the pathway of care
We have developed seven applications - each dedicated to a specific indication - mainly to help healthcare professionals monitor their patients' chronic pathologies. 90% of our activity consists of the regular monitoring of 4,200 heart failure patients. We also provide therapeutic education for them. 220 health centres now entrust us with their patients: They know that we will increase their level of knowledge about this disease and detect periods of risk.
For heart failure, Satelia is 100% covered by the French Social Security. This is relatively new for a "medical device" type application. A hospital or private cardiologist can prescribe Satelia and is paid for the follow-up. General practitioners can also prescribe the application, but for the time being they cannot provide the monitoring themselves.
The use of Satelia is also reimbursed for the 300 French patients with an artificial heart (LVAD - Left Ventricular Assistance Device). This application is the result of a painful experience during an internship: The death of a young patient. Equipped with a LVAD, he suffered a stroke due to an underdose of anticoagulant. He was just below the alarm limit of the device. In hindsight, it was realised that a fine analysis of the parameters could have shown the weakening of the flow, a sign that the pump was clogging. Moreover, patients with a LVAD have a tube that comes out of the abdomen for the rest of their life. The risk of infection is high. Remote monitoring allows regular transmission of photos, which saves the patient from having to travel too often.
We also offer specific solutions for monitoring patients in outpatient surgery, in oncology (chemotherapy monitoring) and for those who have undergone coronary angiography. We also work with a poison control centre in Bordeaux: The application's algorithm aims to assess the level of risk according to the product ingested and any pathologies of the victim, for example if a diabetic child swallows a battery or a type of detergent.
Except for heart failure and LVAD, it is the hospitals that finance the use of Satelia directly, by paying an annual licence to use the application. This may be the case for hospitals that do not have the critical mass to offer such a service themselves, or for establishments that call on us to take over during a given period, such as the summer. Large hospitals are integrating Satelia into their patient pathways as part of their digital strategy: This is the case for Paris Saint-Joseph, in cardiology, or the American Hospital after a coronary angiography.
Digital non-exclusion
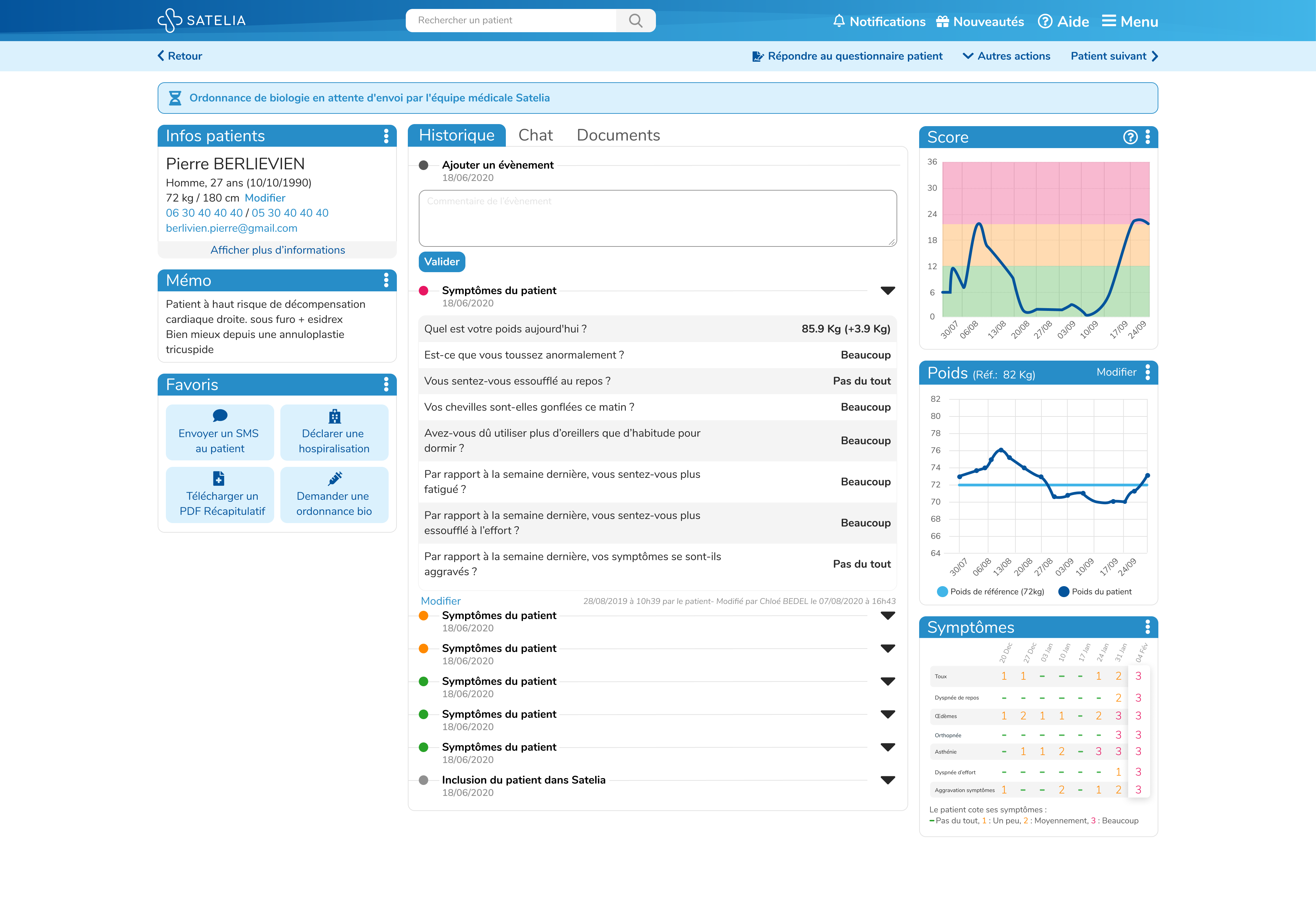
Once enrolled in the programme, the patient receives a regular SMS with a web link. The frequency is defined by the level of risk: For heart failure monitoring, it is one to three times a week. The patient then answers a series of questions about salt intake, sports activity, etc. The information is transferred to the physician, along with a risk analysis performed by a university algorithm based on scientific literature. The physician also receives an alert if a risk threshold is exceeded, e.g. due to weight gain, or if a symptom worsens.
I am convinced that new technologies are only useful if they take into account the reality of the field. 40% of our patients do not know how to use a digital tool. The average age of our patients is 81. We even have a 102-year-old patient. We can always provide them with a connected object, such as an iPad, but this is the best way to make them feel uncomfortable. That's why we prefer to call them, two or three times a week. Technophile patients benefit from remote monitoring and therapeutic education via digital tools; non-technophiles have access via human interaction. In France, we are the only ones to offer such a service, which combines digital and human interaction for prevention and remote monitoring. This allows all patients to take control of their health.
Satelia's 27 specially trained nurses call patients who are not connected to their landline and ask them the relevant questions to feed the algorithm, of which there are currently eight. The call takes about six minutes. It's short, but it's very reassuring for patients. For some, it's the only call they make all week. We can also call our “connected” patients if they have forgotten to fill in the online questionnaire or show insufficient knowledge of an important topic such as spotting emergency signs.
Perspectives
Our start-up was supported from the outset by professionals from the Bordeaux University Hospital. This support was invaluable, particularly thanks to their expertise in cybersecurity. We also had the opportunity to take part in a hackathon, which really boosted Satelia's development.
From an economic point of view, the results are there for Social Security. The analysis needs to be refined, but one euro invested in this remote monitoring solution saves between three and four euros.1 It is still too early to know whether Satelia's effectiveness is homogeneous according to the severity of the patient's condition. But if we don't monitor those who are apparently doing well, we miss the point at which they start to get worse. Some of these patients, if they are not monitored and therefore sufficiently informed about their condition, will not be able to recognise their worsening on their own.
Other applications are being tested, including one dedicated to monitoring kidney transplants. The next step is to obtain reimbursement following a clinical demonstration of effectiveness. In fact, Satelia is developing like a drug: We are moving forward phase by phase, and evaluating the solution at each stage.
Satelia's next big step is its distribution abroad. We have already translated and adapted the interfaces. Several versions are ready: Germany, Italy, United Kingdom, Spain and Portugal, and we are actively looking for partners.
Dr. Nicolas Pagès
You can read the original article in the French languange from our partners at esanum.fr here.
Notes and Sources:
1. Charlotte Puel. La télésurveillance clinique dans l’insuffisance cardiaque : intérêt d’un système de télésurveillance mis en place au centre hospitalo-universitaire de Bordeaux – Sciences du Vivant [q-bio]. 2020
Citations (English version by the translator):
Page 63 : "This is a retrospective observational study conducted at the Bordeaux University Hospital between August 2018 and April 2020. All patients included in the Satelia remote monitoring system from August 2018 to September 2019 were included in the analysis. Patients included in the telemonitoring system were asked to complete a questionnaire twice a week regarding their symptoms and weight. Alerts generated were analysed retrospectively from data available on the secure Satelia site and from patients' medical records (...) 123 patients were included during this period, with an average follow-up time of 10.5 months."
Page 85 : "When a patient presented signs and/or symptoms of cardiac decompensation that generated an alert by the remote monitoring system, and a modification of treatment at home (in the majority of cases an increase in diuretic treatment) allowed a return to the previous state, we estimated that a hospitalisation was avoided. Over the total duration of follow-up, we estimated that 26 hospitalisations were avoided."
