Is Parkinson's disease born in the gut?
Researchers at Johns Hopkins Medicine report having found further evidence that Parkinson's disease originates between cells in the intestine and travels through neurons to the brain.
Experiments in mice show transmission of α-synuclein from the intestine to the brain
Researchers at Johns Hopkins Medicine report having found further evidence that Parkinson's disease originates between cells in the intestine and travels through neurons to the brain. The study, described in the June issue of the journal Neuron, offers a new, more accurate model in which to test treatments that could prevent or stop the progression of Parkinson's disease.
Made in collaboration with our partners from esanum.it
Parkinson's disease is characterized by the accumulation of misfolded α-synuclein in brain tissue. The formation of Lewy bodies compromises a person's ability to move, think or regulate emotions.
A recent study conducted by the Johns Hopkins University School of Medicine has sought to deepen knowledge related to the development of the disease. The new study is based on observations made in 2003 by the German neuroanatomist Heiko Braak, who demonstrated the presence of poorly folded α-synuclein accumulations even in enteric neurons of patients with Parkinson's disease. There is a great deal of evidence to support the strong intestine-brain connection in the onset and development of the disease. Researchers in Baltimore, USA, have suggested that misfolded α-synuclein can migrate from the intestine to the brain through the vagus nerve, which runs from the brain to the abdomen.
To test this hypothesis, the researchers injected 25 micrograms of synthetic misfolded α-synuclein into the intestines of healthy mice. They then analyzed brain tissue from mice one, three, seven and ten months after inoculation. Scholars have thus verified that α-synuclein has spread along the entire path of the vagus nerve, arriving at distribution in the brains of mice.
The researchers then repeated the experiment in mice undergoing surgical denervation, with interruption of the vagus nerve. A seven-month check after the inoculation of α-synuclein in the intestine showed that mice with severed vagus nerve showed any of the signs of cell death found in mice with the intact vagus nerve. According to the research team, denervation stopped the spread of the protein.
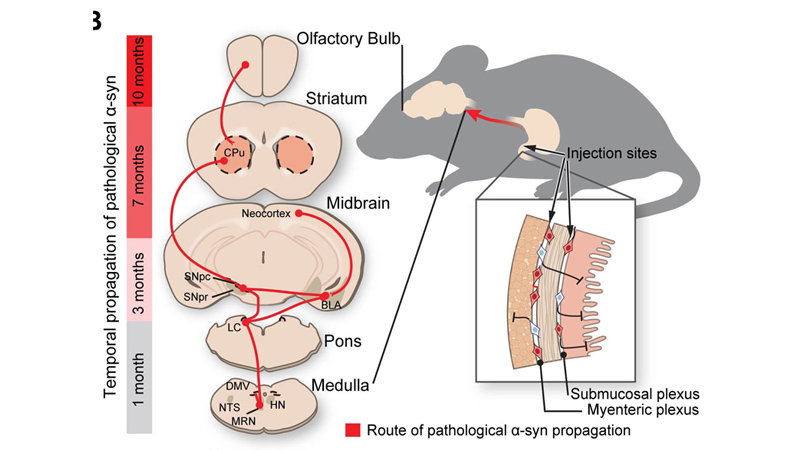
Image Credit: Ted Dawson / Johns Hopkins Medicine
The researchers then investigated whether, in addition to anatomical-pathological differences in the progression of Parkinson's disease, there were also behavioral differences. To do this, they evaluated the behavior of three groups of mice: with an injection of misfolded α-synuclein, with an injection of misfolded α-synuclein and vagus severance, control mice without injection and intact vagus nerves. Researchers examined the activities commonly used to detect signs of Parkinson's disease in mice, namely building burrows and exploring new environments. The seven-month verification from the start of the experiment confirmed that mice with an injection of poorly folded α-synuclein without a severed vagus showed signs of Parkinson's disease.
Overall, the results of this study show that α-synuclein in mice can travel from the intestine to the brain along the vagus nerve and that blocking the transmission pathway could be the key to preventing the physical and cognitive manifestations of Parkinson's disease.
Source: Kim S, Kwon SH, Kam TI, Panicker N, Karuppagounder SS, Lee S, Lee JH, Kim WR, Kook M, Foss CA, Shen C, Lee H, Kulkarni S, Pasricha PJ, Lee G, Pomper MG, Dawson VL, Dawson TM, Ko HS. Transneuronal Propagation of Pathologic α-Synuclein from the Gut to the Brain Models Parkinson's Disease. Neuron. 2019 Jun 17. pii: S0896-6273(19)30488-X. doi: 10.1016/j.neuron.2019.05.035.