Medical History: Curing illness with illness
Before Sir Alexander Fleming discovered penicillin in 1928, syphilis treatments were nightmarish and included mercury vapors or getting injected with a potentially fatal disease.
Ever since Sir Alexander Fleming discovered penicillin in 1928, a famous STD has been, if not extinct, at least treated with excellent results: syphilis. This was frankly good news, especially given the treatments that were applied before Fleming’s time to those who had the misfortune of catching “Cupid's disease”.
Made by our partners in esanum.fr
In the long list of universal human traits, there is a strong temptation to blame someone else if something goes wrong. There is no escaping this in medical matters, and if there is one disease that makes you aware of it, it is syphilis.
All over the world, the names given to it over the centuries reflect the desire to make it clear that it's still the fault of some other person. Charles VIII's French soldiers were quick to describe it as the "mal de Naples" or "mal Italien" when they returned from Campania at the end of the 15th century, at the time of the Italian Wars. Mirroring this, the Italians spoke of it as the "mal francese".
It was the same for the United Provinces (anxious to emancipate themselves from the Spanish Netherlands): the "venereal plague" could then only be Spanish, just as it was obviously Polish for the Russians.1 One guesses here a real little geopolitics of the infection, between possible routes of contamination and prejudices against the “foreigner”: eternally guilty and inevitably sick.
All but one, in fact. Yes, but which one?
Mercury vapors
To the credit of those who had the unpleasant surprise of waking up one morning with bad news at the bottom of their underwear, the "great pox"2 is... ugly. Not so much in its first stage, when it is unpleasant but still limited in its discomfort. The star of venereal diseases then confines itself to the appearance of infectious cankers located exactly where you don't want to see any, namely on the genitals and in places where the bacteria responsible, Treponema pallidum3, has entered the body. This can also include the lips, mouth, or tonsils, with a rather obvious display.
It is in the later stages when things get truly unpleasant. When untreated, syphilis causes migraines and recurrent joint pain, but above all the appearance of skin lesions all over the body, a sort of small, pale pink, or pronounced red spots on the mucous membranes and on the genitals in particular. It was not by chance that one of the first steps, during the times of widespread anxiety in busy brothels, was a scrupulous examination of the client's genitals by the sex workers themselves.
In the third stage, a few years later, things could turn into a nightmare: the disease attacks the organs and flesh, sometimes to the point of disfiguring the patients. Some see their noses literally collapse and are forced to wear prostheses.
Artificial nose, 17th or 18th century
Symptoms are not just about appearance. Syphilis is a disease that can lead to serious neurological complications: meningitis, paralysis, stroke, epilepsy, deafness, dementia of all kinds, and other conditions that lead straight to a fatal outcome in the most aggressive forms: a death that is severely painful.
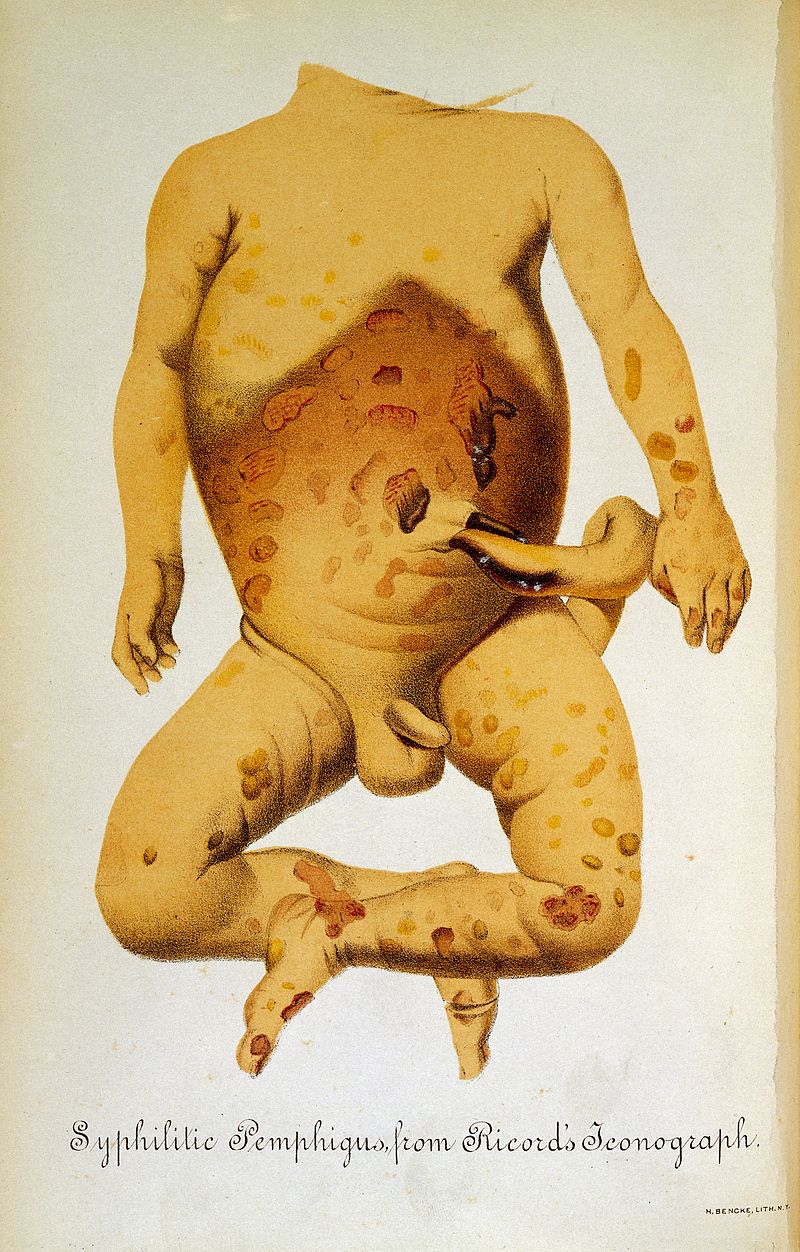
Newborns also suffered the disease (image: circa 1883)
Faced with the frightening damage of syphilis, which was considered even more terrible than leprosy when it began to spread in Europe around 1495, medicine struggled with it for a long time. From the mid 16th century and for at least 300 years, the main therapeutic response recycled an ancient remedy used to treat skin diseases: mercury.
It was applied by all means: plasters, frictions, fumigations (or "mercurial perfumes"). Not only does it not work, but the remedy is worse than the illness: mercury, especially when inhaled by the patient, causes hallucinations and dizziness, plunges patients into frightening mental states, and triggers a cascade of side effects, such as gum irritation and tooth loss.
As soon as the Austrian physician Julius Wagner-Jauregg decided to properly tackle the problem in a thorough manner in the aftermath of WWI, there was quite a crowd in his waiting room.
Malaria to the rescue
Wagner-Jauregg was a psychiatrist and neurologist by training, but his main interest was in soldiers who were deeply affected by the fighting during and after the 1914-1918 conflict. At a time when no one yet was talking about post-traumatic stress, Julius was betting on electroshock. The practice did not have the wind in its sails in public opinion, which considered it barbaric. It was even said that the soldiers treated by Wagner-Jauregg preferred to go back to the front than to stay in his clinic.
For, in fact, Wagner-Jauregg's way of working was... questionable, to put it mildly. An example? Convinced that masturbation was one of the causes of schizophrenia, Wagner-Jauregg had decided to prevent some of his young psychotic patients from indulging themselves by sterilizing them without their consent. These practices caused the physician some legal problems, from which he escaped unharmed, thanks in part to the friendly support of Sigmund Freud.
Wagner-Jauregg, a neurologist, treated syphilis patients in the advanced stages of the disease: the brain was affected and the paralysis well established. And he made a curious observation. Somewhat by chance, he finds that those of his patients who develop a high fever then get much better. It doesn't take him long to draw a very logical conclusion: it is enough to provoke high fevers to obtain a therapeutic gain.
All that remained was to provoke the fever in question. After several unsuccessful attempts, Wagner-Jauregg took in a patient suffering from malaria in his clinic. And the good news is that in 1917 malaria was cured with quinine. Wagner-Jauregg concluded that he could cure the then intractable syphilis by inoculating his syphilitic patients with malaria. Once their physical condition would improve, he would follow the treatment with quinine. It was, in his view, literally a matter of treating evil with evil, or more precisely with fire: this "malaria therapy" invented by Julius Wagner-Jauregg was also called pyrotherapy (from the Greek pyros, fire).
Consent? What consent?
The first tests were rather conclusive: six of the nine syphilitic patients to whom Wagner-Jauregg inoculated malaria saw their condition improve significantly after seven to ten feverish episodes. And good for them, even though the physician never bothered to ask their opinion.
We find this practice ethically mind-boggling today. From a medical point of view, however, the studies that have been carried out in the wake of this, confirm Wagner-Jauregg's intuition that malaria therapy works in at least one out of every two cases.
These results were more than enough for Wagner-Jauregg to win the Nobel Prize for Medicine in 1927. The Nobel academy did not seem to care too much about the fact that 15% of patients treated in this way died not of syphilis... but of malaria. This was the end of an era: the idea that desperate diseases justified desperate treatments was only really challenged at the end of the Second World War, in the wake of the trials of Nazi physicians in Nuremberg, Germany.
In the short term, the prestigious prize won by Wagner-Jauregg had an effect: pyrotherapy (also known as malaria therapy) became widespread throughout the world for two decades, until penicillin, discovered in 1928, became the real cure for syphilis. It was not until 1974 that the last few syphilitic patients4 stopped being given malaria, 34 years after the death of Dr. Wagner-Jauregg, whose ideas and troubling medical practices still prove polemic in his native Austria.
France, 1926
Notes:
1. Translator’s note: See Bahar Gholipour’s article on the illness: “The Italians called syphilis the French disease, the Japanese called it the Portuguese disease, the Turkish called it "the French or Christian evil," and the Persians called it the Turk evil."
2. Author's note: As opposed to "smallpox", also known as variola, pox, and the red plague. Some of the skin symptoms resemble those of syphilis, at least in the early stages.
3. Author’s note: Discovered in 1905 by two German scientists, Fritz Schaudinn and Erich Hoffmann. Under the microscope, it looks like an old remnant of a tagliatelle noodle with butter.
4. Book (In French): Michel Caire, Soigner les fous. Histoire des traitements médicaux en psychiatrie. (Nouveau Monde éditions - 2019)