Vaccines and climate change: between prevention and mitigation
Global warming will favour zoonotic diseases, and populated areas risk becoming hotspots. Vaccine development is crucial; so is their supply and access.
Translated from the original Italian version.
The effects of climate change on vaccine-preventable diseases
Climate change poses an unprecedented threat to mankind. It will be a major challenge in the 21st century and will be the cause, according to an estimate by the World Health Organisation, of around 250,000 deaths per year by 2030, mainly in the lowest income countries.
Although the direct and indirect consequences of climate change on human health are multiple and far from fully explored, a growing body of evidence demonstrates its potential to exacerbate the frequency and spread of communicable infectious diseases.
The narrative review Mitigating the effects of climate change on human health with vaccines and vaccinations summarises the available evidence on the effects of climate change on vaccine-preventable diseases.
The study examines the direct effect of global warming on water-related diseases such as cholera and other enteropathogens, helminth infections and leptospirosis. It also explores the outcomes of rising temperatures on vector-borne diseases such as dengue, chikungunya and malaria, and the impact of temperature and humidity on airborne diseases such as influenza and respiratory syncytial virus infection.
We provide next some summaries from the introductory part of the review, the three chapters addressing specific aspects, and the authors' conclusions.
Changes in temperature and precipitation, overpopulation, and infectious diseases
Climate change is a major driver of infectious disease dynamics through changes in temperature and precipitation: alongside diseases with a significant global impact, other infectious diseases are expected to emerge and re-emerge, especially in low- and middle-income countries.
A recent study of 375 infectious diseases worldwide found that 58% were exacerbated by climate change through numerous pathways, particularly vector- and water-borne diseases and by bringing pathogens closer to people. Furthermore, global warming is expected to alter the geographical distribution of mammals and humans and thus facilitate the sharing of pathogens, as there will be an increasing overlap in the distribution of species.
This could lead to the emergence of potentially pandemic zoonotic diseases, similar to the spread of HIV and SARS-CoV, on humans made possible by the spillover of wild hosts: for example, bats have been identified as important facilitators of possible future viral sharing. In particular, areas of high human population density are expected to emerge as future hotspots for these events, highlighting the impact of human interference on altering ecological habitats.
Mitigating climate change-related infectious disease threats through mitigation strategies will require significant long-term efforts and time to achieve impact. While measures to address climate change and its impact currently focus on economic and social policies, the potential role of vaccines as a mitigation strategy has been little explored.
The discovery of immunisation and the subsequent development of vaccines for previously life-threatening infectious diseases have already saved millions of lives worldwide. Vaccines have become an indispensable tool in recent decades to prevent and control infectious diseases, as seen recently during the COVID-19 pandemic.
The above review examines the main vaccine-preventable infectious diseases associated with climate change, the stages of vaccine development for these diseases, and their challenges.
Climate-sensitive and vaccine-preventable diseases
Almost all pandemic-risk and high-impact infectious diseases are being studied by vaccine developers. While vaccines are available to prevent major childhood infectious diseases, vaccines that prevent other high-impact infectious diseases have yet to be developed.
Table 1 summarises vaccine-preventable (or possibly vaccine-preventable) diseases associated with climate change and illustrates the status of vaccine development for selected conditions.
Specifically considered in the narrative review are:
- food- and water-borne diseases
- vector-borne diseases
- tick-borne infections
- air-borne infectious diseases.
Prevention and mitigation: the role of vaccines and vaccination
The coming decades will be marked by the disruptive and destructive consequences of global warming, including the exacerbation of climate-sensitive infectious diseases, which pose a serious global threat to human health.
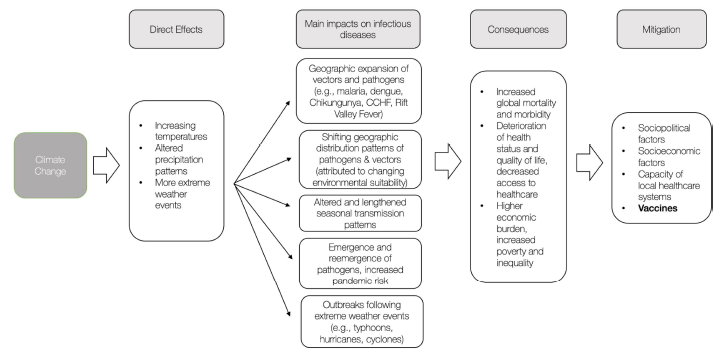
Figure 1 presents a summary of the impact of rising temperatures and the resulting mitigation factors. Taking action to prevent and mitigate potential consequences is crucial. The review focuses specifically on vaccines against cholera, yellow fever, malaria and dengue.
The way forward: developing vaccines for a changing climate
The Intergovernmental Panel on Climate Change (IPCC) has recognised the potential of vaccines in mitigating the effect of climate change on vector-borne diseases, along with surveillance and warning systems. However, multiple challenges remain to fully exploit vaccination as a global strategy, mainly related to vaccine development, supply, access and delivery. It will be necessary to:
- adopt vaccination strategies to combat climate-sensitive diseases.
- prepare for possible pandemics.
- increase the supply and delivery of vaccines.
- combat vaccine hesitancy.
Conclusions
Although still limited, evidence is accumulating on the impact of climate change on infectious diseases, an impact confounded by related covariates, including mitigation measures, geographical distribution and variations within countries. Important non-climate determinants of disease transmission, such as globalisation, public health systems and socio-economic conditions, could also be indirectly affected by rising temperatures and should be addressed simultaneously.
Two issues are relevant: prevention and mitigation
Further research and monitoring in the form of large-scale longitudinal studies are needed to better understand the health effect of climate and environmental changes as they are constantly evolving. Meanwhile, collaborative surveillance activities are also essential measures to improve predictive models and epidemic preparedness, while guiding global and local policies for the introduction and prioritisation of vaccination schemes.
Developing vaccines to mitigate the impact of climate change
Currently available vaccines should be distributed to achieve wider coverage, especially in low- and middle-income countries. Whether single vaccines should be developed for specific diseases or combination vaccines are questions that need to be urgently addressed by stakeholders and developers.
Considering the potentially severe effects of climate change on infectious diseases, the resilience of the health sector should be strengthened. In this context, global vaccination strategies can serve as an important mitigation tool and must become a priority for research and development, procurement, and delivery.